What Is a Patellar Tendon Rupture? Causes, Symptoms & Treatment Explained
A patellar tendon rupture is not the kind of knee injury you can “walk off.” One moment your knee feels normal, and the next you may not be able to straighten your leg, climb a step, or even stand without the knee giving way.
Many people notice sudden pain at the front of the knee, swelling that builds quickly, and a feeling that the leg has lost its support.
In this blog, you will learn what a patellar tendon rupture actually is, the most common patellar tendon tear causes, the signs that suggest a ruptured patellar tendon, and how doctors confirm the diagnosis.
Understanding the Patellar Tendon
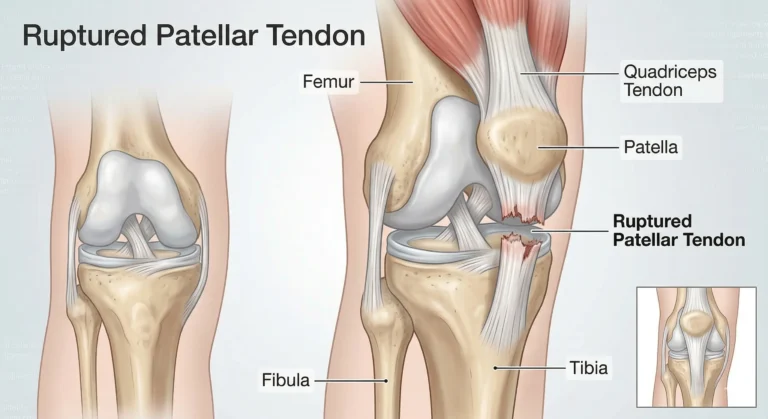
The patellar tendon is a tough band of tissue that runs from the lower edge of the kneecap to the top of the shinbone. It plays a central role in how the knee works.
When you straighten your leg, stand up from a chair, walk upstairs, or push off the ground to jump, this tendon is carrying force from the thigh muscles towards the lower leg. When it is healthy, these movements feel smooth and controlled. When it is injured, even simple actions can become difficult or impossible.
When this tendon tears completely, the knee loses its ability to extend. This is why a ruptured patellar tendon is considered a disabling injury that almost always requires surgical repair.
What Causes a Patellar Tendon Rupture?
A healthy patellar tendon is extremely strong. A rupture usually occurs when high force meets a tendon that is either overstressed or already weakened.
Common patellar tendon tear causes include
- Sudden, forceful tightening of the thigh muscles, such as when landing awkwardly from a jump or pushing off suddenly
- A direct blow to the front of the knee, often caused by a fall, collision, or impact injury
- Sports that involve repeated running, jumping, or sudden changes in direction, particularly basketball, football, and volleyball
Factors that weaken the tendon
- Long-standing patellar tendinitis, often called jumper’s knee
- Repeated micro-tears that never fully heal
- Corticosteroid injections near the tendon
- Chronic medical conditions like diabetes, kidney disease, rheumatoid arthritis, or lupus
- Use of anabolic steroids or long-term oral steroids
In rare cases, both knees can be affected at the same time, a condition known as bilateral patellar tendon rupture, which is often linked to underlying systemic disease or medication use.
Symptoms of a Ruptured Patellar Tendon
A complete rupture usually announces itself clearly. Patients often describe a popping or snapping sensation followed by intense pain just below the kneecap.
Typical signs include
- Immediate swelling and bruising at the front of the knee
- Inability to straighten the leg or perform a straight-leg raise
- The knee giving way when trying to stand or walk
- A visible or palpable gap below the kneecap
- The kneecap sitting higher than normal due to loss of tendon attachment
Partial tears may cause pain and weakness but still allow some knee extension. They require a careful assessment to avoid progression to a full rupture.
How a Patellar Tendon Rupture Is Diagnosed
Diagnosis begins with a focused clinical examination. Difficulty extending the knee is a key finding.
Imaging studies help confirm the diagnosis and assess the severity:
- X-rays may show the kneecap pulled upward in complete ruptures
- MRI scans provide detailed views of the tendon, showing whether the tear is partial or complete and identifying associated injuries
Prompt diagnosis is critical as delayed treatment can allow the tendon to shorten and scar, making repair more difficult.
Treatment Options for Patellar Tendon Rupture
Treatment is planned as per the size of the tear, functional loss, and patient factors such as age and activity level.
Non-surgical Treatment
Small partial tears may sometimes be managed without surgery. This approach typically includes:
- Knee immobilization in full extension
- Crutches to limit weight-bearing
- Structured physical therapy to restore strength and motion
Close monitoring is essential. When function does not improve, surgery may be required.
Surgical Treatment
Complete ruptures usually require surgery to reattach the tendon to the kneecap. Early repair offers the best outcomes and lowers the risk of long-term weakness.
During surgery, the tendon is secured using strong sutures or anchors, carefully tensioned to restore normal kneecap position. In chronic patellar tendon rupture, where the injury is old, graft tissue may be needed to lengthen or reinforce the tendon.
Patellar Tendon Rupture Recovery Time
Recovery is gradual and requires commitment to rehabilitation.
General Recovery Timeline
First 6 weeks
During the early healing phase, the knee is protected in a brace to keep it stable. Movement is limited, and weight-bearing is carefully controlled, often with the support of crutches. This period allows the repaired tendon to heal without excess strain.
6 to 12 weeks
As healing progresses, gentle knee movement is gradually introduced. Supervised physiotherapy focuses on restoring the range of motion and beginning light strengthening exercises, particularly for the quadriceps muscles.
3 to 6 months
Rehabilitation becomes more active. Exercises now focus on rebuilding muscle strength, improving balance, and retraining the knee for everyday movements such as walking longer distances, climbing stairs, and light functional tasks.
6 to 12 months
Patients slowly return to higher-level activities, including sports or physically demanding work, depending on their progress. Strength, coordination, and confidence in the knee continue to improve during this phase.
Most patients regain good overall knee function. However, full strength and endurance can take up to a year, especially for those returning to sports or heavy physical activity.
Long Term Outlook and Possible Complications
With timely surgery and consistent rehabilitation, many individuals return to work, routine daily activities, and recreational sports. Some degree of stiffness or mild strength difference between the legs can remain, particularly if treatment was delayed.
Possible long-term issues include reduced knee motion, persistent weakness, or, in rare cases, re-rupture of the tendon. These risks are higher in untreated injuries or in chronic patellar tendon ruptures where surgery was postponed.
Care Under Dr. Guillermo Sanchez
Treating complex knee injuries requires careful judgment and precise planning. Dr. Guillermo Sanchez brings extensive international experience in orthopedic surgery, sports-related injuries, and trauma management.
Why Trust Dr. Guillermo Sanchez?
- Extensive international orthopedic experience- Trained and practiced across leading hospitals in Europe and the UK, bringing globally aligned standards of care to every case.
- Expertise in complex knee and sports injuries- Skilled in managing acute, chronic, and high-impact tendon injuries with a clear focus on restoring strength and function.
- Personalized, patient-centered treatment planning- Every treatment plan is customized to your anatomy, activity level, and recovery goals, not a one-size-fits-all protocol.
- Emphasis on safe surgery and structured recovery- Combines precise surgical techniques with carefully planned rehabilitation to support reliable healing and long-term knee stability.
His approach prioritizes accurate diagnosis, timely treatment, and rehabilitation that reflect each patient’s daily demands and long-term goals.
By combining proven surgical techniques with structured, closely guided rehabilitation, his focus is on restoring mobility while reducing the risk of long-term limitations.
Moving Forward After a Patellar Tendon Rupture
If you are experiencing sudden knee pain, weakness, or difficulty straightening your leg, early evaluation is essential. Timely care can make the difference between a smooth recovery and lasting impairment.
Book an appointment with Dr. Guillermo Sanchez to address any knee issues for a pain-free life.
