How Diabetes Affects Foot and Steps to Prevent Diabetic Foot?
Diabetes mellitus is a complex chronic condition that affects nearly every system in the body, and its impact on the lower extremities is particularly severe. For individuals managing diabetes, diabetic foot issues are not just minor inconveniences; they represent a significant, potentially life-altering risk.
As a specialist in orthopedic surgery here in Dubai, Dr. Guillermo Sanchez frequently consults with patients whose diabetes has led to complex foot complications. Dr. Guillermo Sanchez’s goal is to educate, treat, and empower our patients to protect their mobility and overall health.
This comprehensive guide explains how diabetes can cause diabetic foot issues, details the warning signs, and outlines the critical steps necessary for effective diabetic foot care and prevention.
The Double Threat: How Can Diabetes Cause Diabetic Foot Issues?
Diabetes causes damage to the feet through two primary and interconnected mechanisms, both driven by persistently high blood sugar levels:
1. Diabetic neuropathy (Nerve damage)
High glucose levels are toxic to the nerves, especially those farthest from the spinal cord (in the feet and legs). This nerve damage, known as neuropathy, is the main reason for many diabetic foot symptoms.
Loss of sensation: The feet lose the ability to feel pain, heat, or cold. A patient might step on a sharp object, wear a shoe that is rubbing, or develop a blister without ever noticing the injury. This loss of protective sensation allows minor injuries to progress unchecked.
Foot deformity: Neuropathy can cause the small muscles in the feet to weaken, leading to structural changes such as claw toes or the severe collapse of the midfoot, known as Charcot Foot. These deformities create abnormal pressure points, drastically increasing the risk of wounds.
2. Peripheral artery disease (PAD)
Diabetes also damages the blood vessels, causing them to narrow and harden (atherosclerosis).
Poor circulation: Poor circulation in the feet and legs severely limits the delivery of vital oxygen, nutrients, and immune cells, making it difficult for wounds to heal. Even a small cut can take months to close, and an infection can rapidly become severe and widespread.
These two factors, an inability to feel an injury (neuropathy) combined with an inability to heal an injury (PAD), create the dangerous cycle that defines the diabetic foot problem.
Recognizing Diabetic Foot Symptoms
Vigilance is the most powerful tool in preventing severe complications. You must know how to know if you have cartilage damage in the knee when looking for diabetic foot symptoms every day. Early warning signs include:
Numbness or tingling: A pins-and-needles sensation, especially in the toes, or a complete loss of feeling.
Burning pain: A persistent, uncomfortable burning or cramping sensation, often worse at night.
Skin changes: Visibly, the skin may be dry, cracked, and appear shiny or discolored. Hair loss on the feet and lower legs is also common.
Temperature changes: Feet may feel abnormally cold or hot.
Swelling: Persistent or excessive swollen feet diabetes can indicate a severe problem, such as infection, inflammation (like Charcot foot), or poor venous return due to circulatory issues.
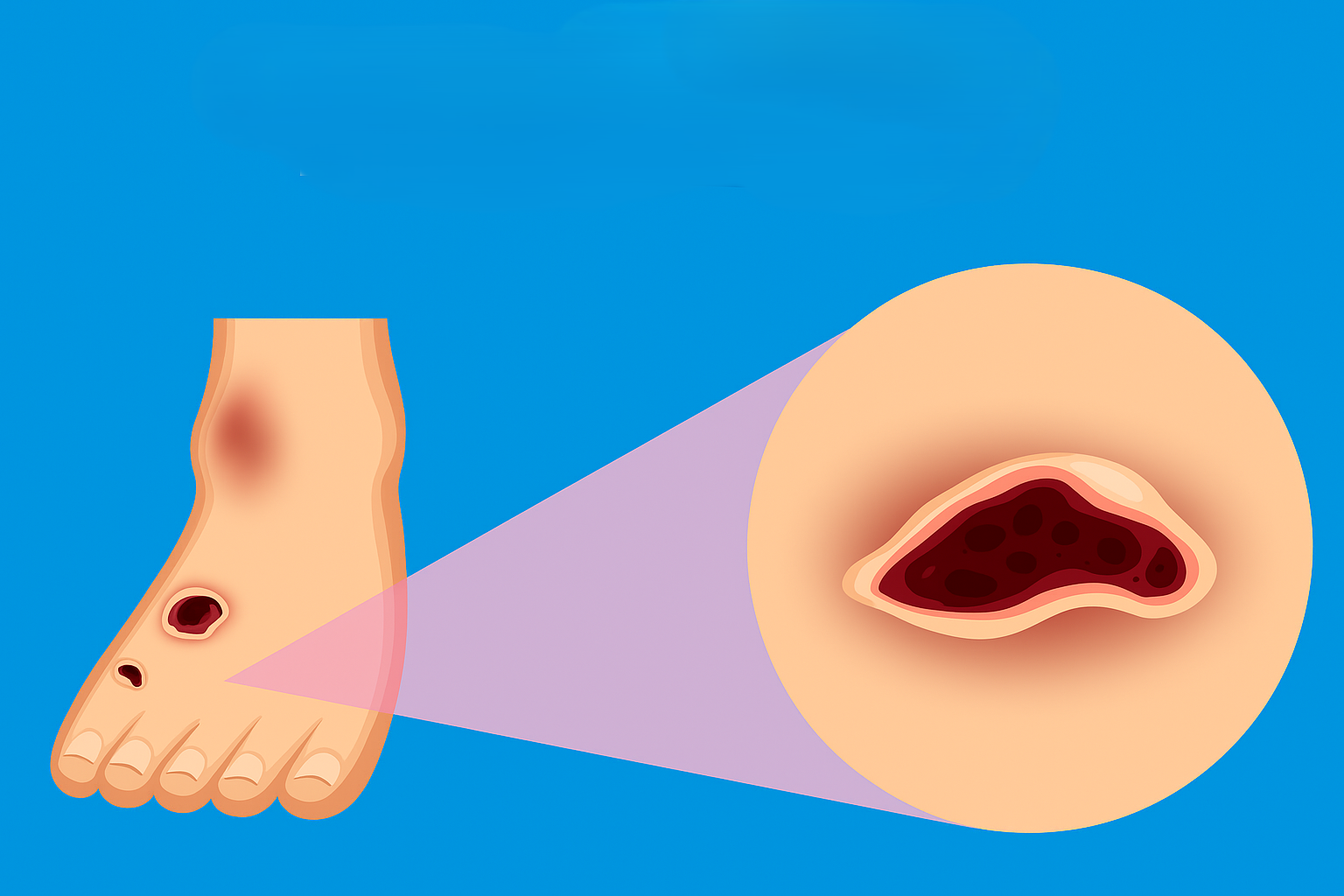
The ulcer: The most critical sign is the presence of a diabetic foot ulcer any break in the skin, blister, or sore that does not heal within a few days.
If any of these diabetic foot symptoms are present, immediate consultation with a specialist is required.
The Danger of the Diabetic Foot Ulcer
The most serious complication of diabetes in the foot is the diabetic foot ulcer. Because of neuropathy, these ulcers are typically painless, allowing them to go undetected for weeks or months, often worsening until the underlying bone becomes infected (osteomyelitis).
An ulcer is essentially an open wound that typically appears on the skin, most frequently found under the balls of the feet or on the big toe.
Due to poor circulation, the infection can quickly spread, and if the blood supply is too poor for antibiotics to reach the infected site, the risk of partial or total amputation becomes alarmingly high.
Prevention is Key: Essential Diabetic Foot Care
The cornerstone of diabetic foot treatment is prevention. Strict, daily diabetic foot care can dramatically reduce your risk of developing severe complications.
Inspect feet daily
Check your feet thoroughly every day top, bottom, sides, and between the toes. Use a mirror if you cannot see the bottoms easily. Look for cuts, blisters, red spots, swelling, or ingrown nails.
Wash feet daily
Wash your feet every day in lukewarm water. Crucially, dry them completely, especially between the toes, to prevent fungal infections.
Moisturize
Moisturize the tops and bottoms of your feet to avoid cracking, but it's crucial to skip the area between the toes to prevent the growth of fungus.
Trim nails properly
Trim nails straight across, never rounding the corners, to prevent ingrown toenails. If you have poor sensation or circulation, have a podiatrist or specialist perform this task.
Always wear shoes and socks
Never walk barefoot, even indoors. Wear clean, dry, white cotton socks that wick away moisture. Ensure your shoes fit perfectly they should be comfortable immediately, with no breaking-in period.
Regular check-ups
Schedule regular foot examinations with your diabetic care team.
When to Seek Specialist Diabetic Foot Treatment?
If you discover a cut, blister, or diabetic foot ulcer, do not attempt to treat it yourself with home remedies.
You must cover the wound with a clean bandage and contact your physician immediately. Should the issue require specialized intervention, Dr. Guillermo Sanchez, as an orthopedic surgeon focusing on the lower extremities, offers essential expertise in:
Wound debridement: Surgically cleaning the diabetic foot ulcer to remove dead tissue and promote healthy healing.
Correction of deformities: Surgically correcting bone deformities, such as those caused by Charcot foot, to eliminate abnormal pressure points that cause new ulcers.
Infection management: Working with infectious disease specialists to treat deep bone infections and prevent amputation. If your diabetes is affecting your feet, proactive intervention is non-negotiable.
Contact Dr. Guillermo Sanchez today. Dr. Guillermo is dedicated to delivering the specialized care you need to safeguard your feet and preserve your mobility.
